Understanding Parkinson’s disease, the symptoms it causes, and how the condition can affect movement, balance and everyday life.
Parkinson’s disease is a progressive neurological condition that affects how the brain controls movement. Symptoms often develop gradually and may include tremor, slow movement, muscle stiffness and balance problems. Learning to recognise these changes can help individuals and families understand the condition and seek the right support.
- ✔ Common symptoms of Parkinson’s disease
- ✔ Early signs and movement changes
- ✔ Causes and risk factors
- ✔ How Parkinson’s disease progresses over time

What is Parkinson’s Disease?
Parkinson’s disease is a progressive neurological disorder that affects the nervous system and the way the body controls movement. It develops when specialised nerve cells in a part of the brain called the substantia nigra gradually become damaged or die. These brain cells normally produce dopamine, a chemical messenger that helps coordinate smooth and controlled muscle movement.
As dopamine levels fall, communication between different parts of the brain becomes disrupted. This leads to the characteristic movement problems associated with Parkinson’s disease, including tremor, muscle stiffness and slow movement. Parkinson’s belongs to a group of conditions known as movement disorders because it primarily affects how the body moves and maintains balance.
Inside affected brain cells, abnormal protein deposits known as Lewy bodies can develop. These deposits interfere with normal brain function and are a recognised feature of Parkinson’s disease. Although Parkinson’s mainly affects movement, it can also cause a range of other symptoms affecting sleep, mood, thinking and the autonomic nervous system.
Symptoms of Parkinson’s Disease
Parkinson’s disease is a progressive movement disorder affecting the nervous system. Parkinson’s disease symptoms develop gradually over time and can affect both movement and other body systems. The most recognisable Parkinson’s symptoms relate to movement, although many people also experience a range of non motor symptoms. The common early symptoms of Parkinson’s disease may be subtle and vary from person to person. Support from specialists in neurological physiotherapy can help people better understand how these symptoms affect movement and everyday activities.
Motor Symptoms (Movement Symptoms)
Motor symptoms are the most recognisable features of Parkinson’s disease. These primary motor symptoms occur because the brain’s control of muscle movement becomes disrupted as dopamine levels fall.
- ✔ Slow movement (bradykinesia)
- ✔ Muscle stiffness or rigidity
- ✔ Tremor, often starting in one hand or arm
- ✔ Balance problems and postural instability
- ✔ Reduced arm swing while walking
- ✔ Changes in posture and movement coordination
Non-Motor Symptoms
Parkinson’s disease can also cause non motor symptoms that affect other parts of the body and nervous system. These symptoms may appear before movement changes or develop as the condition progresses. Common non motor symptoms include sleep problems, fatigue, pain, changes in mood such as depression or anxiety, and difficulties affecting other body systems such as bladder function.
Fatigue is a particularly common symptom and may be linked to sleep disturbances, reduced activity levels or changes within the nervous system.
- ✔ Sleep disorders and REM sleep behaviour disorder
- ✔ Fatigue and reduced energy
- ✔ Low blood pressure when standing (orthostatic hypotension)
- ✔ Changes in mood such as anxiety or depression
- ✔ Difficulty swallowing or changes in speech
- ✔ Excessive sweating or temperature regulation problems
Early Symptoms of Parkinson’s Disease
Parkinson’s disease often develops gradually, and the early symptoms can be subtle. Many people first notice small changes in movement, coordination or everyday activities. These early signs may appear months or even years before the condition is formally diagnosed.
In the early stages of Parkinson’s disease, symptoms may affect only one side of the body. Because the changes are often mild at first, they can easily be mistaken for normal ageing or fatigue. However, recognising early symptoms can help people seek medical advice sooner and better understand what is happening in the body.
- ✔ A slight tremor in one hand or arm
- ✔ Slower movement during everyday tasks
- ✔ Reduced arm swing while walking
- ✔ Muscle stiffness or subtle changes in posture
- ✔ Changes in handwriting (often becoming smaller)
- ✔ A softer voice or reduced facial expression
Not everyone experiences the same early symptoms, and the condition progresses differently for each person. If these changes are becoming more noticeable or affecting daily activities, it may be helpful to discuss them with a healthcare professional.
Looking for Physiotherapy Support for Parkinson’s Disease?
Many people living with Parkinson’s disease benefit from specialist neurological physiotherapy to help maintain movement, balance and independence. Our experienced physiotherapists provide personalised rehabilitation programmes designed to support mobility, confidence and everyday function.
Walking Problems and Freezing of Gait in Parkinson’s Disease
Changes in walking and balance are common symptoms of Parkinson’s disease. As the condition affects the brain’s control of movement, many people experience slower walking, reduced arm swing and difficulty initiating movement. Postural instability and balance problems may also develop over time, increasing the risk of falls.
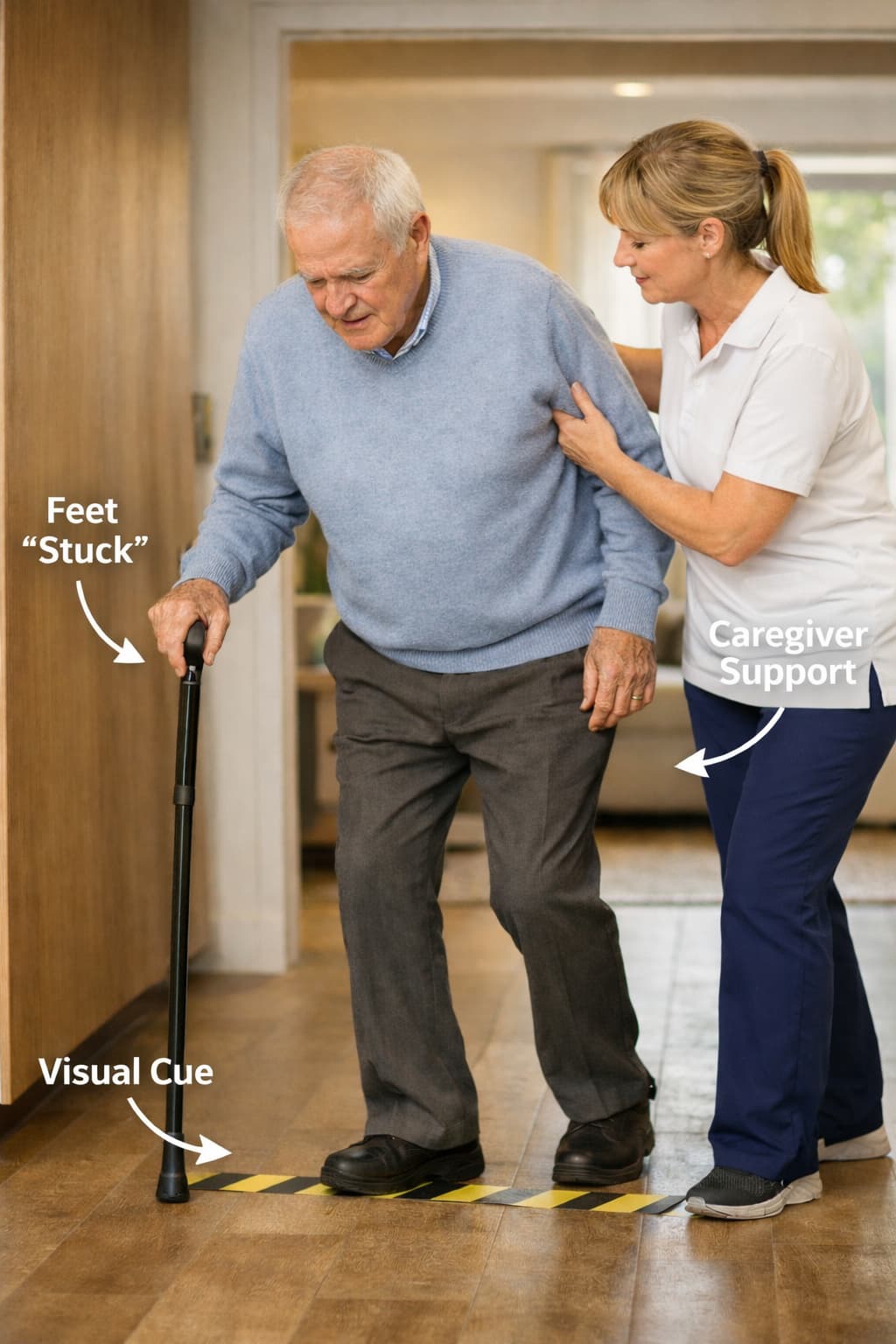
One of the most recognisable walking difficulties associated with Parkinson’s disease is freezing of gait. This occurs when a person suddenly feels as though their feet are “stuck to the floor”, making it difficult to start walking or continue moving. Freezing episodes are more likely to occur in certain situations, such as turning, walking through narrow spaces, approaching doorways or when feeling rushed or distracted.
Understanding the triggers for freezing of gait can help people develop practical strategies to manage it. Techniques such as visual cues, rhythmic movement or focusing on stepping targets may help restart movement and improve walking confidence.
Causes and Risk Factors of Parkinson’s Disease
The exact cause of Parkinson’s disease is not fully understood. Parkinson’s disease is a progressive movement disorder that develops when specialised nerve cells in the brain that produce dopamine gradually become damaged or die. Dopamine is an important chemical messenger that helps regulate movement, coordination and muscle control. As dopamine levels fall, communication within the nervous system becomes disrupted, affecting movement and leading to the movement symptoms associated with Parkinson’s disease.
Researchers believe that Parkinson’s disease is likely caused by a combination of genetic and environmental factors. In most cases there is no single identifiable cause, but certain factors may increase the risk of developing the condition.
- ✔ Increasing age, with most people developing symptoms after the age of 50
- ✔ Genetic factors or family history of Parkinson’s disease
- ✔ Environmental factors that may affect the nervous system
- ✔ Changes within brain cells, including the presence of abnormal protein deposits known as Lewy bodies
Although these factors may increase risk, it is important to remember that many people with Parkinson’s disease have no clear risk factors. Research continues to explore how changes within brain cells and the nervous system may contribute to Parkinson’s disease and how these processes affect movement as the condition progresses.
How Parkinson’s Disease Progresses
Parkinson’s disease is a progressive neurological condition, which means symptoms tend to develop gradually over time. In the early stages, symptoms may be mild and affect only one side of the body, allowing many people to continue with everyday activities.
As the condition progresses, movement symptoms such as slow movement, muscle stiffness and balance problems may become more noticeable. Some people may also experience changes in energy levels, sleep, or thinking as the condition develops. However, the rate at which Parkinson’s disease progresses can vary significantly between individuals.
In later stages, additional support may be needed with everyday tasks such as walking, transfers or maintaining balance. Understanding how Parkinson’s disease progresses can help individuals and families plan appropriate support and maintain independence for as long as possible.
Diagnosis of Parkinson’s Disease
Diagnosing Parkinson’s disease can sometimes take time because the early symptoms may be subtle and similar to other neurological conditions. At present there is no single laboratory test that can definitively confirm Parkinson’s disease. Instead, diagnosis is usually based on a combination of medical history, symptom patterns and a neurological examination.
A neurologist will typically assess how the nervous system is functioning by evaluating movement, balance, muscle tone and coordination. They may also ask detailed questions about when symptoms first appeared and how they have progressed over time.
In some cases, doctors may recommend imaging tests such as brain scans to help rule out other conditions that could cause similar symptoms. A trial of Parkinson’s medication may also be used to see whether symptoms improve, which can help support the diagnosis.
Because Parkinson’s disease can progress gradually, people may have regular reviews with their healthcare team so that symptoms and treatment options can be monitored over time.
Living With Parkinson’s Disease
Living with Parkinson’s disease often involves adapting to gradual changes in movement, energy levels and everyday activities. While the condition progresses differently for each person, many people are able to maintain independence and quality of life for many years with the right support and lifestyle strategies.
Everyday Activities
Parkinson’s can affect everyday tasks such as walking, getting dressed, preparing meals or maintaining balance. Planning activities carefully and allowing extra time for tasks can help people manage these challenges more comfortably.
Home Safety and Adaptations
Simple changes in the home environment can help reduce the risk of falls and improve confidence. Removing trip hazards, improving lighting and installing grab rails in key areas such as bathrooms or stairways can make daily life safer and easier.
Support From Healthcare Professionals
People with Parkinson’s disease are often supported by a multidisciplinary team that may include neurologists, physiotherapists, occupational therapists and speech and language therapists. Each professional plays a role in helping manage symptoms and maintain independence.
Support for Families and Carers
Family members and carers often play an important role in supporting someone living with Parkinson’s. Learning about the condition, attending healthcare appointments and encouraging regular activity can help individuals manage symptoms and maintain their quality of life.
When to Seek Help for Parkinson’s Disease
If symptoms such as tremor, slow movement, stiffness or balance problems are becoming noticeable, it is important to speak with a healthcare professional. Early medical assessment can help identify whether symptoms may be related to Parkinson’s disease or another neurological condition.
People already diagnosed with Parkinson’s disease may also benefit from additional support if mobility, balance or everyday activities become more difficult. Changes in walking, coordination or confidence can develop gradually, and early guidance can help maintain independence and safety.
Family members may also notice subtle changes such as slower walking, reduced balance or increased reliance on support. In these situations, a specialist assessment can help identify the challenges and guide the next stage of support safely.
If you would like to learn more about rehabilitation options, you can read about our specialist Parkinson’s physiotherapy service below.
Frequently Asked Questions
Clear answers to common questions about Parkinson’s disease, its symptoms, causes and how the condition affects everyday life.
What are the early symptoms of Parkinson’s disease?
Early symptoms of Parkinson’s disease often develop gradually and may include tremor in one hand, slow movement, muscle stiffness, reduced arm swing while walking and changes in handwriting. Some people also notice fatigue, sleep problems or a reduced sense of smell before movement symptoms appear.
What causes Parkinson’s disease?
Parkinson’s disease occurs when nerve cells in the brain that produce dopamine gradually become damaged or die. The exact cause is not fully understood, but researchers believe a combination of genetic and environmental factors may contribute to the condition.
Why do people with Parkinson’s have walking problems?
Parkinson’s disease affects the brain’s control of movement, which can lead to slow walking, reduced arm swing, balance problems and changes in posture. Some people also experience freezing of gait, where the feet temporarily feel stuck to the floor when trying to move.
What is freezing of gait in Parkinson’s disease?
Freezing of gait is a common movement symptom where a person suddenly feels unable to start walking or continue moving. It may occur when turning, approaching doorways or walking in busy environments. Understanding triggers and using movement strategies can help people manage these episodes.
How does Parkinson’s disease progress over time?
Parkinson’s disease is a progressive neurological condition, meaning symptoms tend to develop gradually over time. The speed of progression varies between individuals. Some people experience mild symptoms for many years, while others may develop increasing difficulties with movement, balance and everyday tasks.
Can people live well with Parkinson’s disease?
Many people live active and fulfilling lives with Parkinson’s disease. With appropriate medical care, physical activity and support from healthcare professionals, individuals can manage symptoms and maintain independence for many years.





